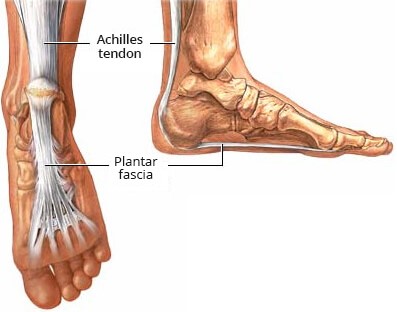
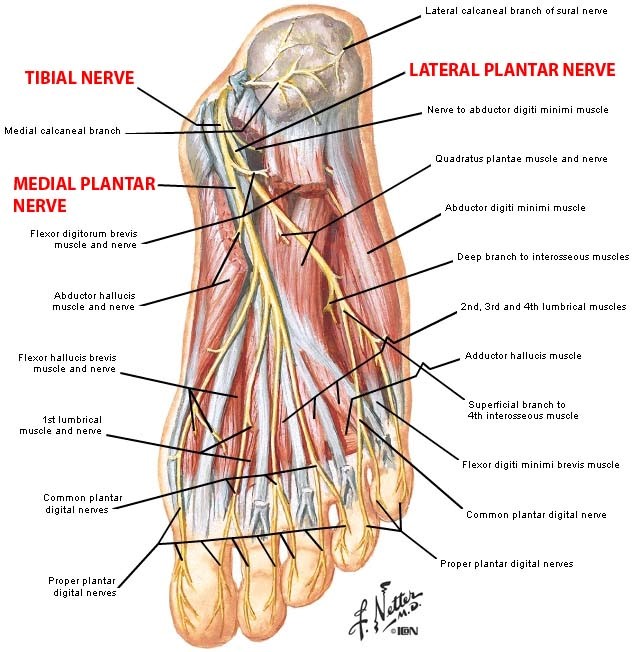
The most common cause of shin splint pain is excessive (in magnitude or duration) of tension on the tibia by the Posterior Tibialis muscle. The reason the pain is so extreme is that the Posterior Tibialis muscle fibers blend with the skin of the Tibia which is called the periosteum. The periosteum has the majority of all sensory nerve endings in the entire bone…so if you are having shin splints, you are having “bone pain” as if the periosteum is tearing…that can be excruciating

Once you understand the job of the Posterior Tibialis you will understand why it hurts and how to facilitate healing. When you walk or run the arch on the inside of your foot lowers with shock absorption impact in a motion termed pronation

The Posterior Tibialis resists this pronation motion much like a shock on a car. So, the more the foot and leg roll inward in both the magnitude and duration…the more “work” demands are placed on the Posterior Tibialis as it resists this collapse of the inside of your foot. The more the Posterior Tibialis works, the more it pulls on the periosteum and the more likely you will have shin pain.
Treatment for Posterior Tibial Shin pain.
- Ice will work as an analgesic…it treats the pain, but doesn’t address the pathology.
- Heat is also an analgesic…it treats the pain, but it may improve circulation to the injured tissue which can bring nutrients needed for healing.
- Anti-inflammatories. They also work as an analgesic and if taken as prescribed will in time reduce inflammation, so once again they do not address the actual pathology.
- Reducing the demand on Tibialis Posterior will lead to true healing of the pathology. Rest can come in several magnitudes…
- Reduce pronation… limit wearing shoes that offer little or no support to the inside of your feet and time walking barefoot.
- Reduce pronation… limit walking on unstable surfaces like sand or gravel.
- Reduce pronation… you can purchase shoes that offer a higher level of motion control and any reputable running shoe store can help you select those.
- Reduce pronation… you can add an arch support to further limit pronation. Feel free to come to Bare Necessities for a free gait analysis to give you advice on both shoe and potential arch support prescription…if you don’t live near Laramie, WY…we are still happy to give you free advice if you can send us video of you walking barefoot on a treadmill. Email to Tony@BarePT.com or send larger files to Anthony.Bare on facebook.
- Reduce Impact… decrease minutes of running or walking. Consider non-impact activities like biking and swimming.
- Reduce Impact… do your walking or running on a treadmill. A good treadmill provides a level and supportive surface.
- Reduce Impact… Reduce running downhill and consider increasing running uphill (once again made easier on a treadmill).
- There is no significant role for strengthening for this pathology… Tibialis Posterior is already over worked…more work is not the answer.
- There is no significant role for stretching for this pathology… the Tibialis Posterior is as tight as it “needs” to be to do it’s job.
- Manual therapy. There is a role for manual therapy to facilitate healing of the Tibialis Posterior and the Tibial periosteum, but if you haven’t addressed #4 above the manual therapy will be much less effective.
While Tibialis Posterior is the most common cause of shin pain, there are other causes and if your symptoms aren’t located on the lower inside of your shin or your pain doesn’t rapidly respond to the treatments suggested above, then it is time to seek medical evaluation.