- Prenatal: There is a whole blog written about Amy’s first two births, but I’ll summarize. Graham was a traumatic inverted “T” C-section and Stella was a home birth VBAC (Vaginal birth after C-section). Both Graham and Stella were well past 41 weeks gestation and over 40 hours of hard labor and 4 hours of pushing during the VBAC birth. I treated Amy’s c-section scar and uterus extensively before conception and during the final trimester I did several sacrotuberous and sacrospinous ligament releases. Juliet was born at 39 weeks 6 days after only 5-6 hours of active labor and less than 20 minutes of pushing. I’m not claiming responsibility for the vastly easier birth, but as a manual therapist it sure makes sense that I contributed. From Amy: I feel like the work that Tony did prenatally made a huge difference. Juliet also engaged in my pelvis prior to labor which was a first for me. My first two births were difficult due to baby’s potitioning and presentation. The assumption (by several medical and birth professionals) is that I had soft tissue restrictions in my pelvis and also scar tissue that prevented optimal fetal positioning and vaginal birth or easy vaginal birth. Having my husband treat both the soft pelvis and scar tissue allowed the baby to get into my pelvis properly and to rotate and descend more easily in labor. As a former doula I have extensive knowledge in optimal fetal positioning, I made it a point to learn as much as I could after my own experiences and I have a great understanding of how the pelvis and baby work during birth. I actually did less to prepare for my third baby than I did my second one as far as optimal fetal positioning techniques are concerned, the biggest difference was the body work that my husband did. One thing that I really appreciated was that Tony and I could speak the same language when discussing the pelvis concerning pregnancy and birth and then he was able to take it farther with his visceral treatment knowledge.
- Mastitis: Amy started running a fever a few days after birth and sure enough I palpated a rigid quadrant in her right breast. I treated the area 5 times over the next 2 days and combined with Ibuprofen, ice packs and cabbage leaf compresses she had complete resolution of her symptoms in 48 hours without having to drag Juliet and herself to the acute care clinic for antibiotics. From Amy: On the 3rd day postpartum I started feeling feverish and having chills. I didn’t notice any hardness or swelling in my breast right away but when Tony palpated he felt the blockage and soon it was hard, engorged, red, warm and very painful. I felt as though I had the flu. We gave ourselves a deadline of 48 hours for improvement or we’d go in. After Tony treated my breast the first time I could tell it was better. The pain was less and it was less engorged. Treatment the first time was pretty painful but each time after it felt better. By our 48 hour deadline it was as if I had never had mastitis at all. My fever peaked at 102.7 (while taking Tylenol) but I was able to stop taking Tylenol completely and it didn’t return. The engorgement and redness was gone and there was no pain. I took ibuprofen for an additional 24 hours.

- Uterinitis: I’m not sure what her diagnosis would have been, but her symptoms included a deep pressure and fullness and a “prolapse” sensation along with feeling “crampy”. On palpation I could definitely appreciate the fullness of the uterus which I treated using visceral therapy techniques with resolution of all symptoms following one treatment. Amy: The only way I could describe what I was feeling was to use the word prolapse. It just felt heavy and full in my lower abdomen and even in the top of my vagina. I did look “down there” to see if I could see anything since sometimes prolapse after birth can happen and it can be bad enough for the cervix or even uterus to fall into the vagina but I’m happy to report that at 2 weeks postpartum I looked completely normal and pre-baby in the lady area. I didn’t tear during the birth and really had very little swelling so healing was fast externally but I was really glad to see nothing coming out either. I’ve been doing a ton of kegels every day but after the first time Tony treated my uterus that heavy feeling went away. I did pass some small clots after that treatment but my bleeding is pretty minimal and after the second treatment I had no more clots. I didn’t really want to talk to him about this issue, I am still his wife and want to maintain some level of sexuality and since he had already watched me push the baby out I didn’t want to become “clinical” to him but I realized if I were going to talk to anyone about it, it should be him. He was the most likely to help me and he did. I’m still not 100% sure that I don’t have some prolapse. My pelvic floor is pretty weak and even before this pregnancy I had a lot of incontinence when I sneezed and especially when I run. I still want to do some pelvic floor rehab with a PT that specializes in it but I want to continue to have my husband treat me externally until I start going.
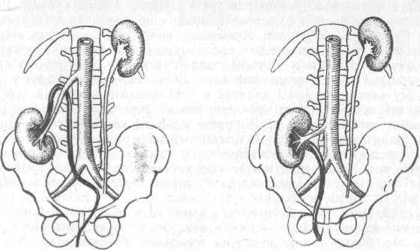
- Kidney Ptosis: Amy developed left flank pain which was worse when laying supine, with change of positions and breathing. I examined and did some treatment on her ribs, but they really felt fine. When I palpated her left kidney her symptoms were aggravated. The left kidney certainly makes sense for two reasons… 1.) In late term pregnancy the baby spends most of her time on the left side of her mom’s body 2.) There is a genitourinary vein that drains the uterus and ovaries to the left kidney that isn’t duplicated on the right side. This extra fascial structure would tend to drag the kidney inferiorly once the uterus retreats that direction after birth. I treated Amy’s kidney using visceral therapy and had complete resolution of her symptoms in one treatment. Amy: I had sharp shooting pains in my back that had me doubled over and in tears. I thought I’d broken a rib but I had done nothing to injure myself. The pain was so bad that I might have actually gone in for drugs but instead we got up and Tony treated me at 2am. It immediately felt better and I went from not being able to lay down comfortably to being able to go asleep. The next day it was a bit sore and the next day 100% better. This was about the time I started thinking my husband was a miracle worker. It’s not the first time I or someone else has thought that though.
- Sigmoid dysfunction/constipation: Amy was having unusual pain and difficulty with bowel movements and on palpation the sigmoid colon was clearly the culprit. Once again complete resolution of symptoms following one visceral therapy treatment. Amy: This is another one that I didn’t want to talk about. I don’t like “potty talk” and pretty much avoid that topic with my husband but after two weeks of pretty intense bathroom pain I had to say something. I also felt like I couldn’t talk about the uterine stuff without mentioning this. Basically, every time I had been to the bathroom since I had the baby was super painful. If you’ve ever had a vaginal birth you know that first time going is pretty scary but it didn’t stop being scary. It got more scary because I knew it would hurt. Simple gas hurt. Laying on my back hurt. After two weeks I finally spoke up and things were better the next day after one treatment. He said my colon felt “ropey”. I’m happy to report that all is well and I don’t have to talk about it any more!
Why mention all this? I truly believe that moms are mostly expected to suffer through pregnancy and postpartum pains and difficulties as all part of “being a mom”. Pain and dysfunction are NOT natural states for the human body and I’m a firm believer in giving it a shot manual-therapy-wise. If you are a mom or know a mom recently postpartum, ask her how she’s doing. You may be able to alleviate so much of her pain and birth related difficulties. Trust your hands! Amy: I do think he’s right that as moms we are just expected to have pain and suffer through it. We don’t have to. There’s so much that can be treated and that can feel better.
Lastly, if you are one of those therapists who doesn’t believe in visceral therapy, please contact me! If you are open to the possibility, please attend a course and your practice will never be the same again and you will be able to help so many more people!!
